Photo: Medtronic Strata Valve Photo: Medtronic Strata Valve When I signed up for brain surgery #2, I don't think I understood exactly what I was getting myself into. After all, the strong pain meds administered during my first operation seemed to wipe most of those unfavorable memories from my mind. So, it was a bit of a surprise when I had my first shunt placed a few months ago.* *This post includes graphic images which my be considered disturbing to some readers. Please continue reading at your own discretion. To give you a little background, it took several years for doctors to actually diagnose me with hydrocephalus (see the full story of my late-diagnosis here). In fact, most of my youth was spent looking for answers concerning my status, often regarded as a medical mystery. However, after seemingly endless questions and a prolonged hunt, we finally got our answer and I received the official diagnosis at age 27.
Unfortunately, at this time, I was a little too cognitively impaired (due to growing fluid pressure) to understand the implications when my neurosurgeon first proposed implanting a shunt. Unlike my normal inquisitive self, I did not go home and jump into research. Instead, I scheduled the surgery and hoped for the best. Don't get me wrong, my beyond-wonderful surgeon took good care of me throughout the process (read my full impression of the Houston Methodist neurosurgery team here). However, there is a lot that I did not know about shunts. For one, I had no idea that having a foreign object placed in your body could have so many consequences. Sure, I had a good idea from my previous experience that brain surgery isn't fun - like any other surgery, it means pain of some degree paired with a long recovery. But, boy did I underestimate the results! ...On March 21st, 2018 Dr. Jonathan Zhang placed my first VP shunt: a programable Medtronic Strata Valve.
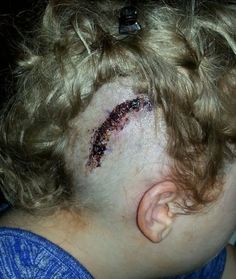
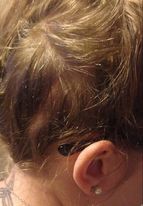
When I first arrived for surgery, it was the typical rundown of paperwork and prep. But then, the nurses wheeled me down for a special CT. I say "special" because before they could scan my head, they cutout several small sections of hair so they could put on these tiny adhesive markers, which act like a strange sort of GPS. These "lifesavers" (so nicknamed by the nurses because of their donut-like shape) then map out the head so the doctor can clearly see what he or she is inserting and where. I thought the technology was pretty neat, but the hydrocephalus had made my scalp extra sensitive (cry when brushing hair worthy) so I was not too fond of the long, hair scraping process they did to prepare the scalp for sticking lifesavers. Plus, we didn't figure out until later that some of the left-behind cutout hair ended up getting really tangled throughout post-op. As you can see in the picture, my hair was so matted that we had to cut some of it out. Thankfully though, they only shaved a small portion for the actual surgery, so most of my hair avoided demolition. Side note: I highly recommend getting a bottle of baby hair de-tangler for the post-op tangles because you will not want to irritate the incision any more than you have to. ...After the surgery, I woke in recovery feeling groggy but otherwise fine. As usual, it wasn't until I was back up in my room and the initial medications wore off that I started to feel much of anything. The pain was dull at first and mostly avoidable as long as I did not lay directly on the wound; however, I found out quickly that it is a little difficult not to irritate the incision.
I remember how hard it was to get comfortable those first few days. I couldn't handle laying on the back of my head because the shunt was placed right behind my right ear. Likewise, I couldn't lay on the sides of my head since both directions caused pain by pulling on the staples used as a surgical closure. And, to top it off, I found that I couldn't lay on my stomach either because of the abdominal suture. Needless to say, I felt as though someone had punched a hole in my head... and they had!
Like my initial surgery (an ETV), I responded with increased sensitivity and stayed in the hospital a week longer than expected. After that, however, I was home and on to the main part of the recovery.
I struggled with severe nausea, vomiting, and headaches for the first several weeks post-op due to continued sensitivity. In fact, I do not remember much of the first few weeks since I was on pain and nausea meds around the clock. But, they helped me get through the worst of it without too much craziness. Blunt honesty provided, it does take some getting used to... Our bodies innately trigger pain signals in the event of a foreign body and shunts are considered just that by our newly baffled brains. And as VP shunts run all the way from the head to the peritoneal cavity (the inside space of your abdominal area), they can sometimes press on little nerves as the tubing shifts. In fact, Mama appropriately dubbed my new shunt Squirrely, since shunts can be pesky little creatures and mine follows suit by being a tad restless at times! But, luckily, the tube is usually tacked down surgically to avoid too much movement - and this is most definitely a wonderful thing! Then, scar tissue eventually forms and better immobilizes shunt tubing so patients likely get some relief - I certainly did. For me, this process took several long weeks but it slowly dissipated to the point that I can now easily bare the occasional twinge I feel when my shunt hits a nerve.
As you have read, shunts most definitely come with a learning curve. There are so many tiny nuances to discover, and the body has to adjust before you can really enjoy the full effects of the improved quality of life offered by the treatment. That said, I hope that this does not stop you from pursuing a shunt as an acceptable treatment option. Of course there are both pros and cons to shunt life (read my list here), but I adamantly agree that there is more benefit than trouble associated with these devices.
With new technology produced every year, neurological patients are now blessed with the reassurance of having viable options that save lives. And these shunts are often programmable, meaning that setting adjustments can easily be made by your neurosurgery care team in-office. Gone are the days of requiring more brain surgery every time you need an adjustment! In fact, I just recently got mine adjusted to drain faster and then back to slower, all with minor changes the nurse made with the help of a small, magnetized remote. Of course, this means that I can no longer come into contact with large-power magnets (like those found in MRIs) without first pre-scheduling an appointment to reset my shunt, but all things considered I would call it a win! ...If you already have a shunt, other readers as well as myself, would deeply appreciate hearing about your experience and what you have learned throughout your shunt life. After all, most of my shunt knowledge came from the informative posts of fellow shuntees after I had the surgery! So please feel free to leave your story and interact with others below.
All of our experience is a bit different, but we grow immensely with the support of others! As always, I appreciate your ongoing support and feedback. Blessings for a happy experience and fellow shuntee love, Dani
If you enjoyed this blog post, please aid us in writing more articles that help readers like you! Answer the short survey below to assist our team in helping more, chronically ill warriors find the helpful stories and information they need to become their own patient advocates! Then, feel free to leave a comment below. We love to hear from our readers!
Pay it forward!
8 Comments
Lisa Aytes
10/6/2018 06:29:53 pm
I met you today at the craft fair. I’m the volunteer that bought the jar with red and white crochet cover. I read your story and am very impressed of your accomplishments. I’ve never heard of what you have but want to let you know that you’re an inspiration. I could tell your parents are very supportive and proud of you. You are a very sweet young lady and I will be following you.
Reply
10/11/2018 08:16:59 am
You are so sweet! Thank you for such wonderful feedback. I cannot even tell you how much this means to us! Reading your comment after our very first show brought tears to my eyes. I hope that you truly enjoy your Christmas jar and we hope to see you at the next show! It was lovely to meet you :)
Reply
Debbie McGreevy
12/11/2019 05:37:39 pm
This is the first blog that was relevant to me so THANK YOU Dani!
Reply
12/11/2019 06:03:40 pm
I'm so glad that my little blog has helped someone, even if only a bit! Just remember that what I write is personal and not to be held as professional medical advice. That said, I would love to help others in any way that I can. Please let me know if there are any questions that I can help answer. I know that the surgeon doesn't always go into detail and waiting for this kind of surgery can be a tad scary.
Reply
10/22/2020 01:53:48 am
Your story is very inspiring for me. Doctor thinks I have Hydrocephalus but I am afraid of surgery. I have dizzy spells, headaches, nausea, fatigue and forgetful. I am a lot older than you as I am 70 yo. My CT suggest hydrocephalus and MRI is inconclusive. So I’m worried. Glad to have read your info🙏❤️
Reply
10/22/2020 12:31:06 pm
Hey Susie!
Reply
hi all my names is Christine im 52 years old . I had planned urgent surgery 6 weeks ago following an incidental find of a large arachnoid cyst at the back of my head . Headache dizziness and nausea and slight neuropathy ed to CT scan . Ihad a cysto peritoneal shunt inserted (CP). i have stumbbled on this site in search of some reassurance . I resonate with Dani s storey evan to to matted hair post op. Iwas discharged from hosp after 1 day ( possibly due to covid situation). I continue with discomforts as described by Dani . My most troublesome issue is the tightness in my neck and find if i dont wear a bra its tighter. will i ever feel better . My shunt is a non programmable device set at medium - no adjustments can be made. I would love to think this shunt may be removed when cyst is drained and perish the thought of further surgery as its been a nightmare so far.I have FU with surgeon in 2 weeks time but informed a probable virtual consult due to covid.
Reply
11/5/2020 07:41:57 am
Christine,
Reply
Your comment will be posted after it is approved.
Leave a Reply. |
AuthorPatient Advocacy Archives
May 2021
Categories
All
|